What is rabies?
Discover our latest podcast
Rabies is a zoonosis, or in other words an infection which can be transmitted from an animal (domestic or wild) to a human.
It is a frightening disease which affects more than 150 countries. According to the World Health Organisation (WHO), rabies kills more than 55,000 people per year across the world, mainly in Africa and Asia. It is thought that 40% of people who have contracted rabies are less than 15 years old.
Causes of rabies
Rabies is most commonly transmitted by coming into contact with an infected animal's saliva, from a bite or serious scratch. Rabies is caused by a virus which is part of the family of Rhabodovirus which can infect any mammal.
Rabies carriers can include foxes, wolves, dogs, cats, badgers, bats or even racoons in America. Dogs are the main hosts and carriers of the rabies virus. Dogs have caused all fatal cases that have been recorded over the years in Asia and Africa. On the other hand, in America, bats were the main culprits for cases of human rabies.
Once the virus has penetrated the body, it starts attacking the central nervous system by spreading along nerves, and eventually reaching the brain and the spinal cord. The incubation period (the time in which the virus remains inside the body) varies a lot depending on the species and the individual: usually, it last between around a few weeks to 3 months but can also last for less than a week or more than a year.
Rabies symptoms
The first symptoms which appear are pain at the site which has been bitten or injured, fever, headaches, nausea, vomiting, and generally feeling ill. Sometimes itching, burn marks or pins and needles can occur. When the virus reaches the brain and the spinal cord, it causes these areas to become progressively inflamed and this is eventually fatal. The former, but less specific symptoms will become much more serious at this point too.
An infected animal will very often display co-ordination problems when it moves, and hypersensitivity of the senses, increased salivation and sometimes muscle spasms in the face. It may also demonstrate abnormally aggressive behaviour which gives it an urge to try to bite anything that comes in its path, but this is not guaranteed in all cases. For humans, the rabies virus will cause similar symptoms.
People who are infected may feel anxious, confused along with major excitement and hyperactivity. They may also suffer from hallucinations, insomnia, and even frenzies. Intense salivation is also usually experienced, with difficulties to swallow, spasms, and a sore throat. At the height of these developments, humans may experience hydrophobia: known as an feeling of extreme fear as soon as you see liquid.
In some cases (around 30%), rabies causes a type of ‘paralysis’, which is characterised by the loss of function in the lower limbs. Once these symptoms appear, death is inevitable and usually takes place between two and ten days after, most commonly from a heart attack. This is why it is so important to respond as quickly as possible after becoming potentially contaminated, to prevent the development of the disease and get the virus out of the body.
Rabies: How to respond after you’ve been bitten?
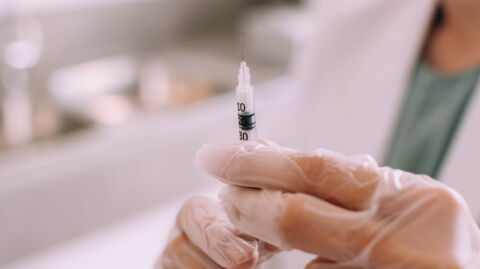
A vet should closely monitor every animal that presents similar symptoms to those of rabies. Likewise, if any animal bites someone, it will be suspected of rabies even if it does not show any signs of the illness. Additionally, immediately after a person is bitten, either seriously or in several places, the wound must be cleaned within 15 minutes with water and soap, and then an antiseptic cleanser.
This will help to get rid of the virus at the infection site, which can reduce the risk according to the WHO. Once the wound has been cleaned, the victim must immediately visit a health centre – here, a doctor can administer an anti-rabies vaccine and if necessary, anti-rabies antibodies. This will depend on the individual circumstances: the type of contact and of course, the animal.
The vaccine is very effective when it is administered in time between contamination and the appearance of the first symptoms. After this point, it is no longer effective in preventing the rabies virus from inevitably progressing.
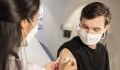
A vaccine to prevent rabies
In order to prevent rabies, it is possible to receive a course of anti-rabies vaccines which are injected before exposure to the virus. They aren’t obligatory but are recommended to travellers who will be spending a lot of time outside or for those who will be spending long periods of time in high-risk areas. People who work in laboratories, vets, or in the vicinity of animals in general are at higher risk of contracting rabies. The vaccination should also be considered for children who live in high-risk areas or are regularly exposed to animals.
The most effective strategy to reduce cases of rabies is to vaccinate animals. The vaccine is strongly recommended for cats and dogs, and obligatory if these animals have travelled from outside the country (proved by a veterinary certificate). In the case of travel, the best thing to do is consult your vets who will explain the vaccination process.
In every case, it is recommended that neither adults nor children feed wild animals and to keep a safe distance from them. If an animal appears to show signs of rabies, it should be immediately reported. Nowadays rabies is a disease that you have to report if you have any suspicions.