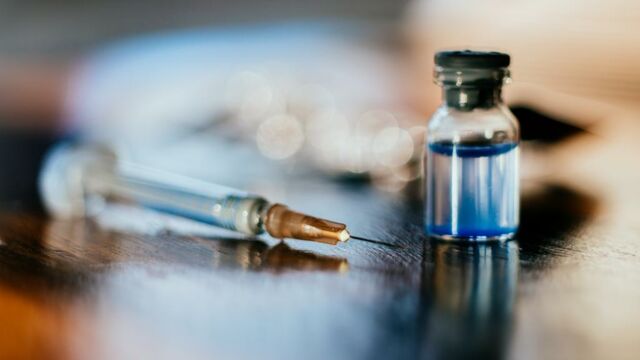
For people with diabetes in developing countries, getting vital daily doses of insulin has gone hand in hand with having access to electricity. Once a vial is opened, the manufacturers recommend storing it in the refrigerator until its expiration date, which is usually after 4 weeks. But an estimated 470 million people worldwide do not have access to electricity and refrigerators for food and medicine, making it difficult to store insulin at home.
Discover our latest podcast
Today, a new program could help revolutionize treatments around the world. It started in the Dadaab refugee camp in northern Kenya, where temperatures can reach 37°C and many do not have access to refrigeration. As a result, patients' lives are pretty much revolving around coming and going to the hospital to receive insulin. Having diabetes can thus mean missing school or work, especially since the camp curfew limits when it is possible to travel.
Insulin could be stored outside of a refrigerator
When the doctors working in the camp noticed that more and more patients were coming to the hospital with complications from their diabetes, they contacted researchers at the University of Geneva and decided to monitor the storage of home insulin in the camp, which experienced temperatures far higher than label recommendations.
The researchers recreated in the laboratory the daily temperature of the camp, which varied between 25 and 37°C, and tested the effectiveness of the insulin. They also studied leftover insulin from vials that patients used after storing them at home. They found that even without refrigeration, the insulin stored in the camp's tropical temperatures could be used safely for four weeks—a revelation that could change the lives of diabetics around the world.
Following their investigation, the team modified the advice they gave to patients, teaching them how to self-inject, check their blood sugar levels and watch for symptoms of danger. Even more exciting, they showed patients how to store insulin at home using a plastic container surrounded by a damp towel. The result was a dramatic drop in the number of diabetic patients presenting to hospital with acute complications. They were able to go to work and school and 'not spend all day looking for medical care to stay alive,' said Philippa Boulle of Doctors Without Borders.
Even though insulin can be damaged when stored at high temperatures, the researchers found that cooler temperatures overnight can keep it safe enough.
Every protein breaks down when heated, but there are proteins that can break down when cooled again, and insulin appears to be one of them.
For now, advice says patients can store their insulin at 'room temperature,' but Leonardo Scapozza, professor at the School of Pharmaceutical Sciences of the University of Geneva, said it should add 'warm settings' for clarity. You'd just need to add three words to that: 'and hot settings,' says Leonardo Scapozza. He added that the findings could also be applied to high-income countries like the United States, for example, during natural disasters and storms that cut off power. Researchers have carried out further studies to test insulin in different climates and are helping refugees from South Sudan bring insulin home.
Insulin storage and diet are key factors in managing diabetes in disadvantaged settings
Today MSF is calling on pharmaceutical companies to change their guidelines and on the World Health Organization to endorse their findings. While many studies have been conducted to test the stability of insulin at different temperatures, the oscillating temperature factor in this study is a 'new turning point,' added Gojka Roglic, WHO physician responsible for diabetes-managing activities.
WHO won't make any recommendations based on this study alone, but Gojka Roglic said it will be included in a review of all research later this year. Ali Bishar, head of MSF's insulin management program at Dadaab refugee camp in Kenya, said diabetes and insulin education is 'paramount' for the program to run smoothly.
After their training, patients have to take a proficiency test. Then they are given their insulin and care is provided in and out of the wards, [...] the program, which started in 2015, has grown from 35 to 45 patients in the past six years.
However, storing insulin is only the start of managing diabetes in low-resource settings. Another major concern is how a poor diet can contribute to the symptoms of patients.
You need to have food when you inject insulin. In some settings, patients fear the injection if they have not taken a meal that day.
Rahmo, who was among the first cohort of patients to start the MSF program in 2015, told Insider that she struggled to get enough and a good diet, but that regardless of her diet, her health had improved. She confided through an interpreter:
Before that, I was confused as to how to move on with my life and if I would survive. Today, I am very happy to be in control of my diabetes at home.