Definition: What Are Hives?
Discover our latest podcast
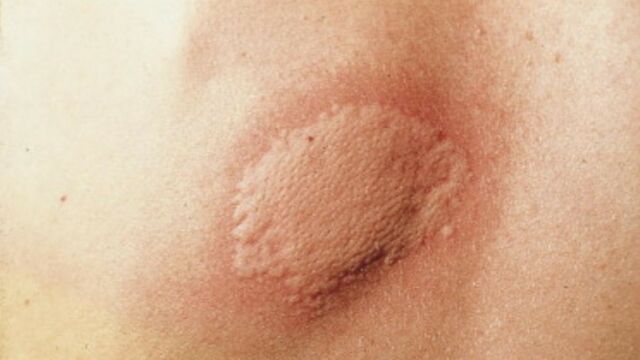
Hives are manifested by an itchy rash and the appearance of red, raised plaques that look like stinging nettle stings. They are also known as urticaria, coming from the Latin urtica, which means nettle.
There are several types of hives:
- acute urticaria, manifesting in short attacks ranging from a few minutes to a few hours, but evolving for less than 6 weeks
- recurrent urticaria where outbreaks of hives reappear regularly at different locations
- chronic hives, characterized by almost daily attacks lasting more than 6 weeks.
Hives are actually more a symptom than a disease. They have various causes and can be associated with other diseases.
Causes Of Hives
Hives occur in response to an external irritant that has been ingested or has come into contact with the skin. Following exposure to this irritant, the body will activate a certain class of white blood cells that will themselves secrete several substances including histamine. This molecule will cause a chain reaction leading to itching and inflammation.
These irritants can be various: they may be food, medicine, cosmetics, insect bites or chemicals. But the trigger element can also be a physical factor such as friction or significant pressure on the skin, such as cold, sun, heat or stress. Everyone is susceptible to hives, however, some factors may make certain people more prone to them. Among these are genetic factors, blood abnormalities, as well as some systemic diseases - autoimmune thyroiditis, lupus and lymphoma, among others.
Symptoms: How To Recognize Hives?
Hives are characterized by an eruption of red, raised bumps, accompanied by itching. There can be a large eruption or several small ones. The rash is often enlarged and swollen. Inflammation is usually greater around the rash and lighter in the middle. At times, the rash is not limited to the surface of the skin. If histamine and other inflammatory agents are released in the subcutaneous layers, the edema may be more severe and the rash will be painful rather than itchy. This is called angioedema.
Treatment: What To Do In Case Of Hives?
Following the appearance of hives, the doctor will try to confirm the diagnosis by performing a clinical examination. They will also try to discover the cause in order to eliminate it. Treatments aim at relieving the symptoms by acting at different levels. However, acute hives usually disappear of their own accord within a few hours. A treatment may still be prescribed to prevent recurrence, including the removal of known triggers and taking an antihistamine drug for a few days. Antihistamines will reduce symptoms by blocking the action of histamine.
In case of chronic hives, treatment will rely mainly on antihistamines for a variable duration, from at least two weeks to 2 to 6 months. Depending on how the symptoms develop, the doctor may increase the dose, or change the antihistamine. If at the end of 3 months or more, the results are satisfactory and durable, the treatment can be gradually stopped. In cases of Quincke's edema or anaphylactic shock, it is essential to go to the hospital straightaway.